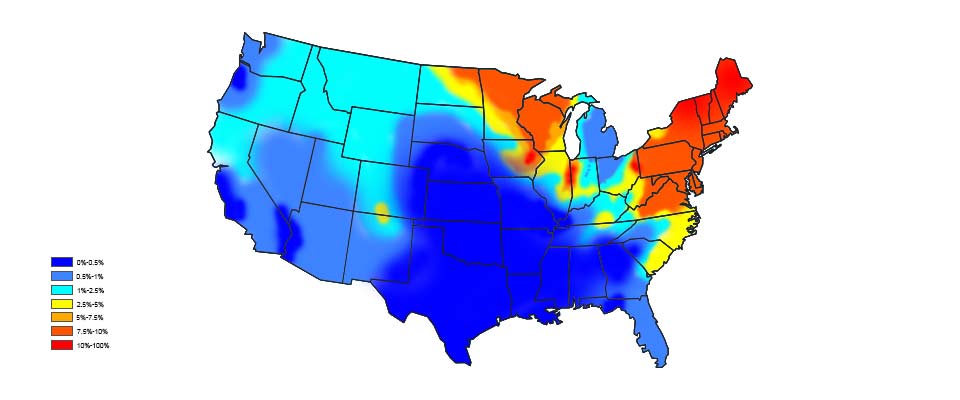
The map above was taken from the Public Library of Science (PLOS). It shows the prevalence of antibodies to Borrelia burgdorferi (a causative agent of Lyme disease) in domestic dogs, an indicator of high-risk areas for humans.
The months of June through September are the time for backyard barbecues and other pleasurable outdoor pursuits. But while you're feasting on burgers and corn on the cob, it's also the most likely time for a Lyme-carrying tick to take a bite out of you (and your pets), according to the Centers for Disease Control (CDC).
Due to a surge in Lyme-carrying ticks this year (a bumper crop of acorns fueled a population boom in the species of tiny mice that ticks feed on), fall 2017 is expected to be the worst on record for new Lyme disease infections.
Where are the high-risk areas?
The highest risk areas are in the Northeast, mid-Atlantic, and upper Midwest. Nearly 95 percent of Lyme disease cases occur in 14 states. Those are Connecticut, Delaware, Maine, Maryland, Massachusetts, Minnesota, New Hampshire, New Jersey, New York, Pennsylvania, Rhode Island, Vermont, Virginia, and Wisconsin. Michigan has also seen a big jump in reported cases of Lyme disease over the last few years.
Live in a high-risk area? Protect yourself by knowing the basics. Ticks live in woody or grassy areas, particularly in moist or humid environments. So, if you find yourself outdoors in these types of places, take some extra precautions:
- Wear tall socks, long pants, sturdy shoes, and a hat
- Avoid going off paths or trails, and stay away from tall grass
- Pair up with a spouse or family member to check each other for ticks (focus on the backs of your knees, ankles, around your hairline, and under your arms)
Want more prevention tips? Learn more at the CDC's website.
Moderate-risk areas?
If you live in states like Ohio, Indiana, or Illinois, you may be in the moderate zone for Lyme disease risk. The same is true for North Carolina, South Carolina, and West Virginia. And remember, although the infection risk on the west coast and in the southern states are lowest risk for Lyme disease, it doesn’t mean the infection is weaker!
Phew! I don’t live in a high-risk area.
Did you go camping or hiking last summer? Visit family or friends who live in wooded areas or have a nice big grassy backyard? If you didn't wear tick-repellent clothing or take other precautions, you’re at risk.
And keep in mind that the geographical range of states that ticks call home is expanding. In fact, the species of ticks that transmit Lyme disease are now found in half of all counties in the U.S.
I don’t remember getting bitten.
Here’s the thing: Often a tick’s bite is painless, and you won't notice it. In fact, about 75 percent of people who develop Lyme disease don’t recall getting bitten. Which makes it more likely that if you were bitten, the tick would stay attached to you for the 36 to 48 hours it needs to set up shop and transmit the Lyme bacteria.
But summer’s over...
Like other infectious diseases, it takes awhile for Lyme antibodies to show up in your blood. Most people will test positive for Lyme starting about four weeks after infection. So the best time to get tested is four to six weeks after you've been bitten (or think you may have been). Getting tested too soon can yield false negative results. If you have any concerns or think you might be at risk, visit your doctor this month.
What are some early symptoms of Lyme?
Some people who've been bitten by a Lyme-carrying tick will get the telltale bull’s-eye rash within 3 to 30 days. But in 30 percent of cases, no rash appears. You may just experience some vague symptoms like a headache, fever, or fatigue, which often go unrecognized for what they are. Click here for a list of early Lyme disease symptoms.
How serious is Lyme if it’s left untreated?
Lyme disease isn’t just an annoyance or a rash that goes away. It can cause severe, long-term nerve, muscle, and joint problems that are very difficult to treat. Some late-stage symptoms include Bell’s palsy (the loss of muscle tone on one or both sides of the face), neck pain that mimics meningitis, joint pain and swelling, shooting or pins-and-needles pain, and heart palpitations. It's a really big deal.
The good news? If properly diagnosed, most cases can be treated with a few weeks of antibiotics. The type of medication you get will depend on your age, allergies, symptoms, and stage of the disease. According to the CDC, 10 to 20 percent of patients who undergo the complete course of antibiotics are left with “Post-treatment Lyme Disease Syndrome,” which manifests as lingering fatigue, pain, or joint and muscle aches.
The best advice? Protect yourself in the first place. Wear insect-repellent clothing that’s been treated with permethrin. Or you can buy a can of permethrin and treat your clothes yourself, though the protection won’t last as long. Also, don’t forget your socks! Apply insect repellent to exposed skin, and, of course, check yourself periodically for ticks.
For more information on Lyme disease, including diagnosis and testing, treatment, and other links and references, click here.